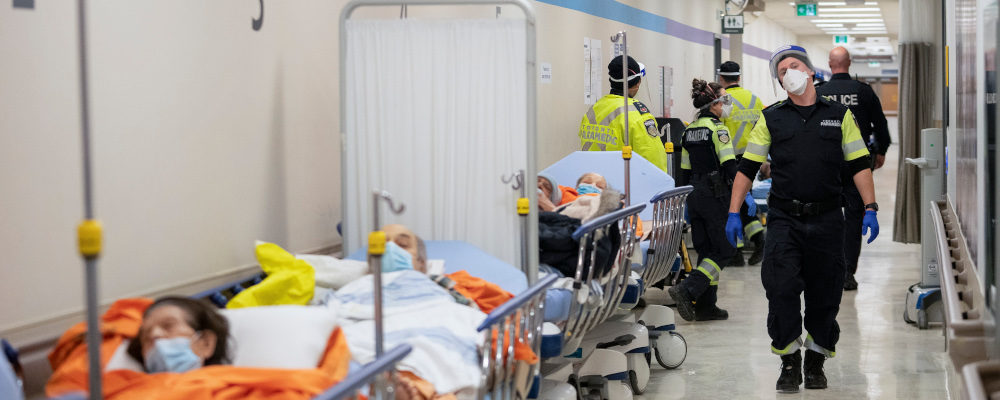
As a previous head of three U.S. cardiovascular organizations, I have always not just defended, but rather promoted, the quality and universality of the Canadian health-care system to my American friends. While our system is universal and generally of good quality, it is far from perfect. Access to care has always been marred by excessive wait times to see a physician, undergo imaging procedures, or have timely surgery.
COVID-19 was particularly hard on our system which already had little flexibility for increased capacity. Despite recent reassurances from government officials, we have a crumbling system that needs urgent crisis management to find both immediate and long-term solutions. We need to stabilize the current mismatch of increased demand and inadequate supply and develop structural and innovative solutions for the future.
While the problem is obvious and needs to be honestly admitted, the solutions are not easy. Governments, used to moving “at the speed of bureaucracy” with options put through a political filter, usually prefer short-term cosmetic fixes rather than fundamental change.
What are our short-term options?
Currently, just as with inflation we have too much demand chasing too little supply. The immediate need is to reduce demand and increase supply, particularly in the most constrained areas of care. Nowhere is this more critical than in our ER crisis. There are too many patients without an alternative to ER care, not enough ER beds, and jammed hospital wards with patients staying too long, especially as they await long-term care beds.
Below are three immediate options to help deal with the problem.
1. Technology. Diagnostic Robotics is an Israeli company that has redefined how individuals access health care using powerful AI algorithms, automated prediction models, and clinical assessment platforms.1Most health execs expect widespread implementation of AI in the next 5 years https://www.businessinsider.com/health-it-leaders-bullish-on-ai-implementation-2020-11 They have been able to successfully reduce ER visits using this predictive technology to determine the urgency of required care and whether it should be provided by alternative options. In 2020, our federal and provincial governments rejected their free offer that I tried to broker to help us triage COVID-19 patients. We urgently need to retain them to work with us now. They can streamline the inflow of ER patients as they have proven in Israel and other countries and meet privacy needs.
2. Increase access to non-emergent care by increased use of Telehealth manned by nurses and nurse practitioners. We also need more 24/7 out-of-hospital urgent but non-emergent care clinics to decant ERs.
3. Adopt U.S. models of bringing urgent care teams to the patient. This has been used successfully to reduce long ER visits, improve care, and lower costs. Dispatch Health in the U.S has a care model that sends emergency care trained teams to patients’ homes with mobile blood work labs, IV fluids, nebulizers, and other ER equipment. In addition, hospital-at-home programs shorten hospital stays and unblock beds for ER patients stuck in hallways. Models such as those used by Johns Hopkins and the Mayo Clinic Acute Hospital at Home model reported in the New England Journal2 Acute Hospital Care at Home: The CMS Waiver Experience https://catalyst.nejm.org/doi/full/10.1056/CAT.21.0338 can be copied. This service provides 24/7 access to a care team of nurses, nurse practitioners, and physician assistants as required. There is also at-home equipment including a telephone connecting directly to your care team, a personal emergency response bracelet, as well as vital sign monitoring devices, internet connectivity, mobile imaging testing, and at-home IV services. There is no reason why we can’t work to adopt this proven, effective approach.
Increase efficiency of health care professionals
Since it takes years to train new practitioners, we need to urgently increase the efficiency of practice and reward those willing to work more. This requires the efficiency of available business models and the use of advanced technology.
1. Increase patient-facing time and reduce clerical tasks. Hospital procedures and newer health information systems increase the amount of soul-destroying nurse and physician time spent on clerical rather than patient-facing time.
2. Open dedicated surgical units outside of hospitals. This can follow the Kensington Opthalmology Centre model that delivers highly efficient cataract surgery as a stand-alone affiliate of the Toronto Western Hospital. We need more of these as well as dedicated orthopedic hospitals so that surgeons with unused capacity have access to more operating time without competing with hospital-based surgeries such as transplants. These dedicated specialized centres maximize surgeon efficiency within a universal care model, at lower cost and higher patient satisfaction. We need them to reduce the unacceptable wait times for low-risk surgeries that are appropriate for such centres.
3. Incentivize care that does not increase burnout. We can do this by maintaining a payment model for appropriate virtual care and providing premium pay for nurses and doctors in high burnout jobs in our ERs and ICUs. We should also now welcome back unvaccinated health-care workers3Unvaccinated health-care workers called back to work after AHS COVID vaccine mandate lifted https://www.cbc.ca/news/canada/calgary/unvaccinated-health-care-workers-called-back-to-work-after-ahs-covid-vaccine-mandate-lifted-1.6385568 as current variants are less dangerous and vaccination status is much less relevant in protecting you from infection.
Increase the number of health care professionals.
Ultimately we need to match increasing medical and nursing school enrolment to high-quality predictive data that defines increasing needs for an aging population and projected higher rates of retirement for nurses and physicians. In the shorter term, we can use foreign medical and nursing graduates under a supervised mentorship program while preserving reasonable regulatory college standards. Some highly trained foreign graduates can be confirmed to be suitable to fully practice within a few months. Others less trained can help out in associate roles much like nurse practitioners.
In 2018, Elon Musk had a crisis on his hands. He had a crucial supply shortage when faced with large numbers of promised deliveries of his Tesla Model 3 that could not be accommodated in his two Fremont California factories already running at full capacity. He simply built a new third production line in a giant tent in his parking lot in two weeks using available scrap material at low cost.
He recognized and admitted that there was a problem and creatively dealt with it in record time. We need governments, unions, medical organizations, and health-care workers to acknowledge that health care is at a breaking point and finally work collaboratively to find solutions that can also be implemented in record time.