The pandemic resulted in an explosion of virtual care that was hampered by the inability to examine or adequately test a patient. The fear of in-person visits and the limitations of virtual care led to missed diagnoses and late presentation of serious illnesses with worse outcomes.
In Israel, during the earlier stages of COVID-19 patients had a box dropped off with contents that would allow for assessment of disease severity and the development of high-risk pneumonia. An oxygen saturation monitor could quickly demonstrate dropping oxygen levels that would require hospital admission. A Bluetooth-enabled stethoscope could be self-applied to electronically transmit heart and lung sounds. This allowed for a triage determination to see if someone with COVID-19 could safely be managed at home, or required hospitalization.
This approach has now been increasingly used for telehealth physician and nurse practitioner visits that incorporate remote physical examinations. It is especially useful for people living in under-serviced areas or when travel is difficult.
Tytocare is a company that has commercialized the concept of providing a comprehensive exam kit that lets you remotely perform guided medical exams with a health-care provider. There is a small Bluetooth-enabled device with attachable plugins such as a stethoscope for heart and lung sounds, a thermal sensor for temperature, an otoscope to look in your ears, and a tongue depressor to look in your throat. The device sends a live audio and video stream to the connected health provider and is designed to provide remote care with patient-guided self-examination.
The ultimate goal of remote care is to provide comprehensive, real-time continuous data on a range of biometric, hemodynamic, and biochemical measurements. Some exciting options currently exist, and others are in the early stages of development.
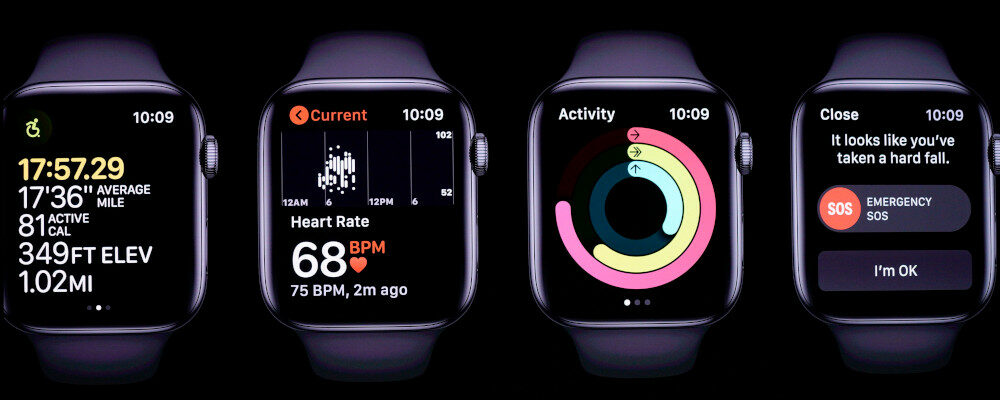
Wearables devices such as the Apple Watch can track your daily steps, oxygen saturation, and heart rate. In my own practice I routinely use it in patients to diagnose heart rhythm disturbances since a high-quality 30-second rhythm strip can be recorded, saved, and transmitted by email. This can determine if the sensed arrhythmia is simply benign extra beats or more serious atrial fibrillation which may require blood thinners to reduce the risk of stroke. An AliveCor device with a finger pad recorder can serve a similar function.
Phone cameras can be used to photograph skin lesions and AI programs used to focus on a particular lesion and differentiate malignant melanoma from benign lesions. As well, wide-field shots can quickly assess a large number of skin lesions and identify which ones may be of concern and require follow-up with a dermatologist.
Home blood pressure monitoring by a validated device is an important way to self-diagnose hypertension and track the success of therapy. Many single reading devices are available; however, newer devices, such as those made by Qardio, can record upper arm measurements over a span of time and provide a trend graph of pressure that can be stored on a smartphone via a wireless Bluetooth connection and then emailed to your physician. These devices should have comparative readings by a health-care professional to confirm accuracy.
Biochemical analysis of interstitial fluid, (that is situated between cells) is an important way to continuously monitor blood sugar in diabetics. The Abbott Freestyle Libre device has a stick-on metal disc with a small plastic, needle-type sensor that sits a few millimetres under the skin and continuously monitors glucose with results sent to a smartphone. Your physician can be allowed remote access to your stored recordings and guide therapy in this unique way. Newer devices can provide alerts for low blood sugar events, as well as being connected to small insulin pumps that titrate the right dose of insulin and avoid serious low blood sugar events.

Sweat is produced by three different kinds of glands, and while it mainly consists of salt and water, it also contains sugars, proteins, and lipids that may reflect our health. Newer technology aims to record blood sugar and other biochemical results by measuring small amounts of sweat. Apple is reported to be working on a sensor recording glucose that will be part of its wristwatch. The opportunities are even much greater than this.
The next generations of wearables being developed will be thin and flexible like bandages that adhere to the skin and move with it. The flexible electrochemical sensor of the future will be able to continuously measure body physiology and track and report dysfunction. There are many challenges to overcome, such as the development of durable materials and power supplies. A number of nanoparticles being tested as sensors and remote batteries carried in your pocket might overcome these obstacles. Potential uses will include the detection of bacterial infection, ions, hormones, and biochemical measures of organ function.
Will the future of medicine include a range of wearable devices that provide early warning of serious disease and monitor the effectiveness of treatment? While we don’t yet know which technologies will work best and be commercially viable, this will likely be our future. The sensors will need to be linked to AI platforms that can analyze the data in real-time and provide both interpretation and alerts linked to the expertise of health-care professionals.
Our current health-care crisis needs these kinds of innovative solutions to streamline care, detect disease earlier, and prevent complications of disease. The combination of a virtual examination coupled with wearable biosensors could lead to earlier hospital discharge and virtual comprehensive follow-up, freeing beds and saving billions of dollars. Biofeedback devices may help us to track our own health and improve fitness.
Canada already has the inventors and data scientists needed for success in this rapidly expanding and important industry. They just need our encouragement and financial support.